What if those persistent, painful blisters that keep popping up on your lips or private areas aren’t just an annoying fact of life, but a direct message your body is desperately trying to send you? For too long, you might have felt trapped by the cycle of tingling, painful sores, and the embarrassment that comes with them, resigning yourself to a fate you thought was unchangeable. But prepare for a game-changer: your body is actually providing clear, actionable signals about what’s truly happening beneath the surface, and unlocking these secrets is your key to real relief and dramatically fewer flare-ups.
The Urgent Truth: Why Ignoring Recurring Blisters Is a Mistake
It’s easy to brush off those persistent blisters as mere “cold sores” or inexplicable “irritation,” but these recurring episodes are actually indicators of a more profound process unfolding within your system. Statistics from leading health organizations like the CDC reveal just how widespread this issue is: more than half of all adults carry the virus linked to oral blisters, and roughly one in six individuals between 14 and 49 years old experience genital involvement. Despite their prevalence, many fail to recognize that this recurring pattern is a critical message. However, common doesn’t mean normal or unavoidable. When these blisters make repeated appearances, your body is actively signaling an underlying condition that demands your focus, not your disregard.
Unmasking the Culprit: How the Herpes Simplex Virus Operates
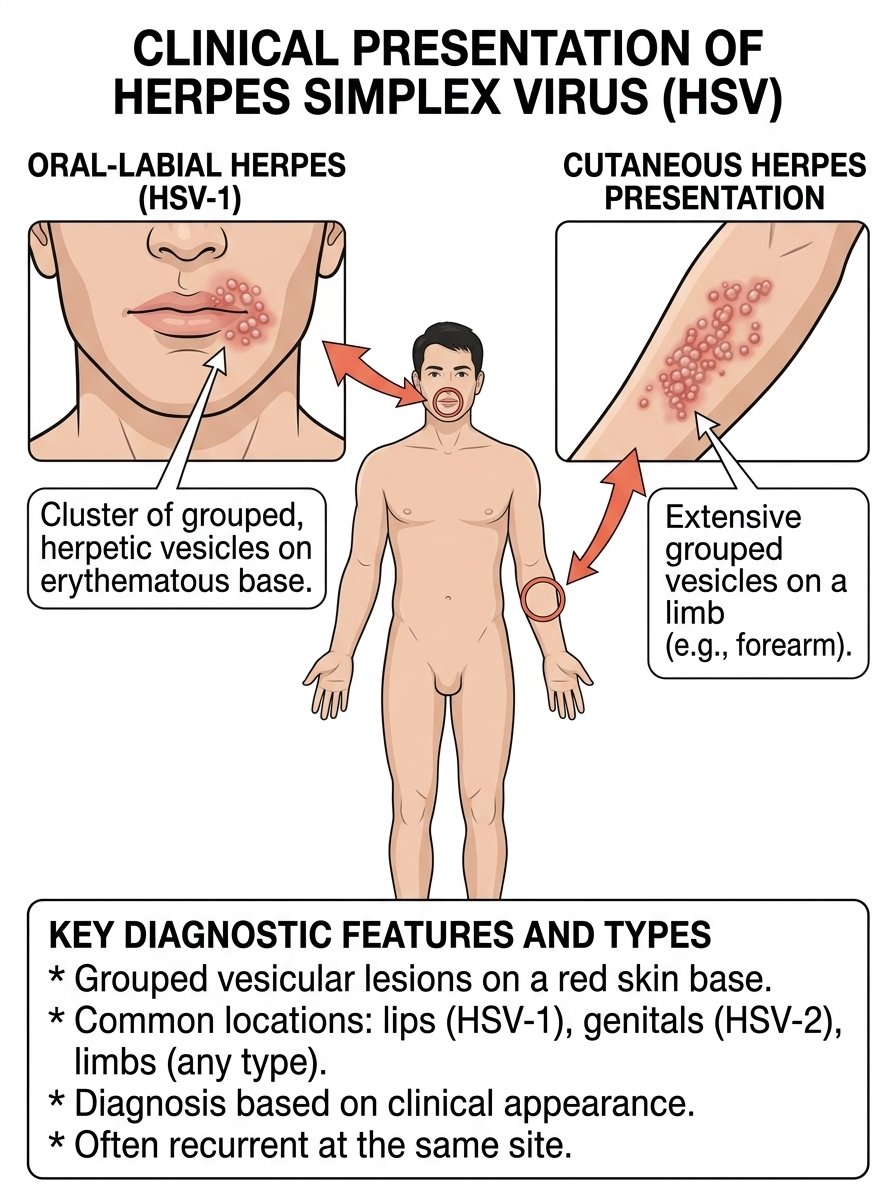
At the root of these frustrating recurrent blisters lies the herpes simplex virus (HSV), which presents in two primary forms. Generally, HSV-1 is responsible for those familiar cold sores that appear around the mouth and lips, while HSV-2 is more commonly associated with outbreaks in the genital region. It’s crucial to understand, however, that both types are capable of infecting either area through direct skin-to-skin contact. Once HSV gains entry into your system, it establishes a permanent residence; it doesn’t vanish. Instead, the virus cleverly retreats into your nerve cells, remaining in a dormant state until a specific trigger prompts its reawakening. Research consistently demonstrates that this reactivation consistently occurs along the identical nerve pathways, explaining why outbreaks so predictably manifest in the exact same locations.
It’s important to clarify that the virus isn’t in a constant state of “attack” within your body. Rather, it patiently bides its time, waiting for an opportune moment to reactivate. Once triggered, those unmistakable blisters can emerge surprisingly quickly, often just hours after you first notice that tell-tale tingling sensation. This intermittent cycle is precisely why the frequency of outbreaks varies so widely among individuals—some may face episodes every few months, while others might enjoy years of reprieve between flare-ups.
Your Body’s Urgent Call: 8 Undeniable Signals It’s Sending
Your body isn’t overreacting; it’s providing crucial insights into its state. Heed these vital messages:
- Active Viral Presence: The virus has established a lasting residence within your nerve cells, making its presence known.
- Immune System Vulnerability: A temporary weakening in your body’s immune defenses has created an opportunity for the virus to reactivate.
- Irritated Nerve Pathways: Outbreaks consistently manifest along the same nerve routes, frequently heralded by that distinctive prodrome—a tingling or itching sensation 12 to 48 hours beforehand.
- Elevated Stress Levels: Scientific research confirms that heightened cortisol levels, often a result of stress, can significantly increase your risk of recurrence, potentially doubling or even tripling it.
- Environmental or Physical Triggers: Exposure to ultraviolet light, such as sunburn on the lips, or physical irritation in sensitive areas frequently serves as a catalyst for the next outbreak.
- Hormonal Imbalances: Many individuals observe that flare-ups coincide with hormonal fluctuations, such as those experienced during menstruation or other cyclical changes.
- Nutritional Deficiencies or Sleep Deprivation: Insufficient levels of essential nutrients like zinc or vitamin D, along with inadequate rest, can compromise your body’s ability to keep the dormant virus suppressed.
- The Crucial Prodrome Window: Recognizing the prodrome phase isn’t just a sign of an impending outbreak; it’s a critical “warning window” that offers you invaluable time to intervene and potentially mitigate the severity or even prevent the full eruption.
But the insights don’t stop with the blisters themselves. These signals are, in fact, an urgent invitation from your body to actively bolster your immune system and effectively minimize triggers, ultimately leading to outbreaks that are both less frequent and significantly milder.
The Hidden Factors: Common Triggers Fueling the Outbreak Cycle
Pinpointing the specific factors that ignite your individual outbreaks represents one of the most impactful strategies you can adopt. Frequently observed triggers include:
- Intense stress or profound emotional exhaustion
- Insufficient sleep, typically less than seven hours on most nights
- Unprotected exposure to direct sunlight
- Significant shifts in hormonal balance
- Periods of illness or a compromised immune system
- Consumption of specific foods rich in arginine (such as nuts or chocolate), particularly if you have a known sensitivity
- Physical friction, often occurring during intimate moments
Diligently logging these potential triggers in a straightforward journal for a few months can often illuminate your distinct patterns—and, crucially, empower you to actively disrupt the cycle.
Immediate Action: Practical Steps to Reclaim Control Starting Today
The encouraging news is that you don’t need to passively await another outbreak to begin improving your situation. Below is a highly effective, practical 90-day strategy that numerous individuals have successfully implemented:
- Consult a Healthcare Professional Immediately – Provide a candid description of your symptoms and inquire about diagnostic testing if necessary. It’s helpful to come prepared with notes on the frequency, duration, and suspected triggers of your outbreaks. Your doctor can accurately identify the cause and explore treatment options, including antiviral medications.
- Master the Prodrome Advantage – The moment you detect the initial tingling sensation, initiate episodic antiviral treatment (if prescribed) to potentially shorten the duration of an outbreak or even prevent its full development.
- Explore Daily Suppressive Therapy – For individuals experiencing frequent episodes, a daily regimen of low-dose antiviral medication has been clinically shown to reduce outbreaks by an impressive 70–90% and significantly lower the risk of transmission.
- Fortify Your Immune System – Prioritize getting 7–9 hours of quality sleep each night, consume a diet rich in essential nutrients, and consider discussing with your doctor the possibility of testing your vitamin D and zinc levels.
- Incorporate Daily Stress Management – Even dedicating just 10 minutes each day to practices like meditation, a brisk walk, or focused deep breathing exercises can yield a noticeable positive impact on your overall well-being.
- Guard Against Trigger Areas – Make it a habit to use SPF lip balm daily and opt for comfortable, non-restrictive clothing to minimize any potential friction in sensitive zones.
The reality is, when you combine expert medical advice with these consistent lifestyle adjustments, the results can be truly transformative. Many individuals report a remarkable reduction in outbreaks, often decreasing from several episodes annually to just one or two mild occurrences.
Your Transformation: A Side-by-Side Look at Life With and Without Management
| Aspect | Without Proactive Management | With Consistent, Empowered Management |
|---|---|---|
| Outbreak Frequency | Frequent, occurring every 1–6 months | Significantly reduced, often 0–2 mild episodes annually |
| Duration & Pain | Prolonged discomfort lasting 7–14 days | Shorter, milder episodes, typically 3–7 days |
| Emotional Impact | Persistent worry, embarrassment, and daily life disruption | Enhanced confidence and a profound sense of peace |
| Transmission Risk | Elevated without protective measures | Substantially decreased through proactive treatment and awareness |
The Bottom Line: You’re Not Isolated, and Lasting Relief Is Within Reach
Ultimately, those recurring blisters on your lips or private areas serve as your body’s candid communication, indicating a clear need for support. By actively interpreting these vital signals, proactively seeking expert medical advice, and implementing modest yet consistent adjustments to your lifestyle, you possess the power to disrupt this frustrating cycle. This path leads to a greater sense of control over your health and a renewed feeling of comfort. Your transformative journey begins with an honest discussion with your doctor and a dedicated commitment to understanding and managing your unique triggers.
Burning Questions Answered: Your FAQs About Recurrent Blisters
1. Will recurrent blisters ever disappear entirely on their own?
While the herpes simplex virus remains a permanent resident in your body, it’s highly common for individuals to experience significantly less frequent and milder outbreaks over time, especially with diligent management. A combination of strategic lifestyle modifications and available medical treatments frequently leads to extended periods completely free of symptoms.
2. Are these recurring blisters exclusively caused by the same virus?
In the vast majority of recurrent instances, yes—the herpes simplex virus is indeed the main underlying cause. Nevertheless, it is crucial to undergo a thorough evaluation by a medical professional. This ensures that any less common potential causes are ruled out and that the most appropriate and effective treatment plan is confirmed specifically for you.
3. What’s the best way to discuss this with my partner without feeling ashamed?
Approaching the conversation with honesty and factual information is generally the most effective method. Emphasize that this is an incredibly common viral condition, openly discuss various protection strategies, and highlight the proactive steps you are taking for management. With open communication, mutual understanding, and appropriate medical support, many couples successfully navigate this aspect of their relationship.
Crucial Disclaimer: This article is provided strictly for general informational purposes and should never be considered a replacement for personalized professional medical advice, accurate diagnosis, or comprehensive treatment. It is imperative to always consult with a qualified healthcare provider for tailored guidance concerning your specific symptoms or health condition. Please be aware that individual outcomes can differ significantly, and prompt professional evaluation is always fundamental for receiving appropriate care.