Imagine waking up every single month to a wave of pelvic pain so intense it radiates through your legs, triggers debilitating nausea, and leaves you utterly exhausted before your day even begins. This isn’t just ‘bad cramps’; it’s a relentless, suffocating cycle that forces millions of women to miss work, cancel crucial plans, and question if their own body is turning against them. For far too long, these agonizing symptoms have been carelessly dismissed as ‘just part of being a woman,’ silently stealing years of vibrant life and peace of mind. But what if there’s a powerful truth waiting to be uncovered? Stay with me, because the knowledge you’re about to gain could finally explain years of mysterious pain, validate your experience, and empower you to reclaim control over your health.
What Exactly Is Endometriosis?
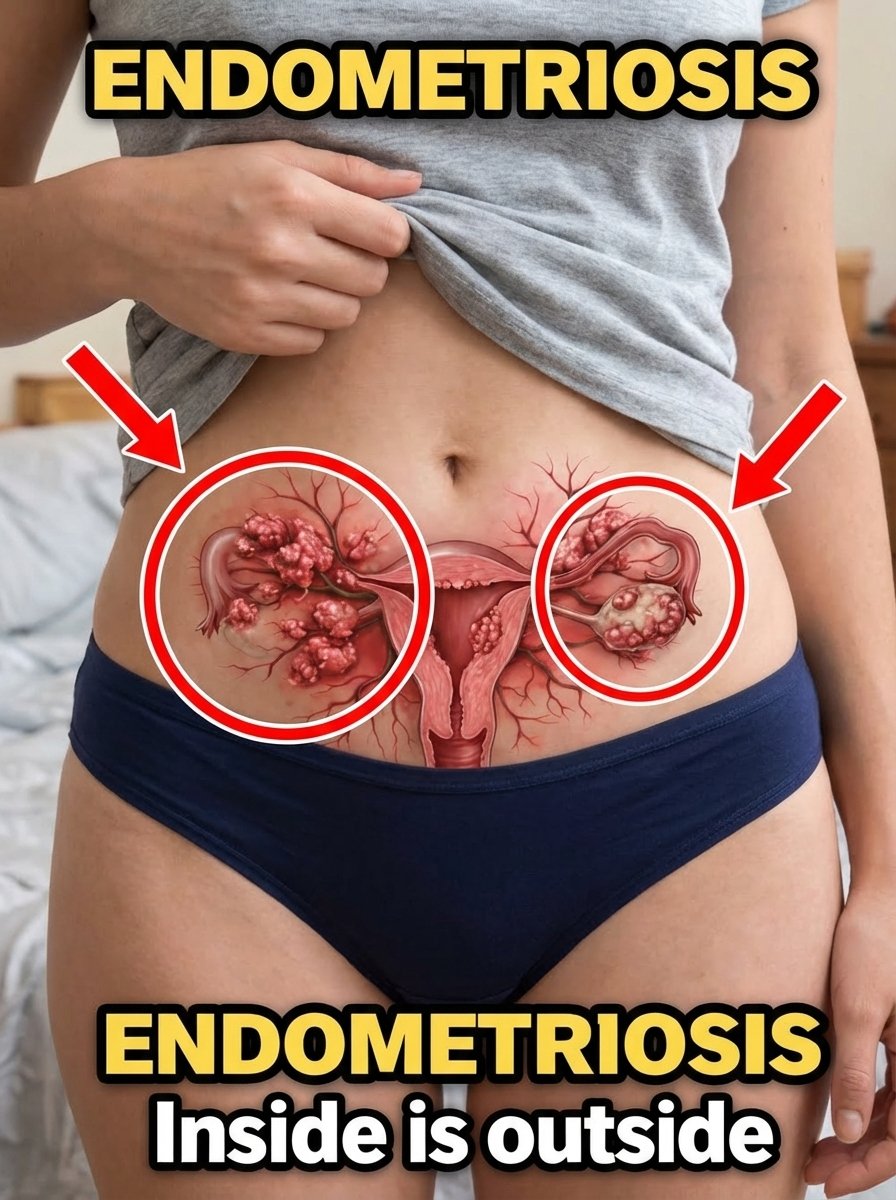
So, what exactly is this elusive condition? Endometriosis is a chronic disorder where tissue remarkably similar to the lining of your uterus (the endometrium) begins to grow *outside* of it. This rogue tissue frequently appears on organs like the ovaries, fallopian tubes, the exterior of the uterus, and can even spread to the bowel and bladder. Here’s the critical part: each month, this misplaced tissue reacts to your hormonal cycle just like your uterine lining does—it thickens, breaks down, and bleeds. But unlike regular menstrual blood, this internal bleeding has no escape route from your body. The devastating consequence is persistent inflammation, painful scarring, and the formation of adhesions that bind organs together, leading to intense, often debilitating pain.
But here’s a startling fact that often goes unacknowledged: endometriosis is far more widespread than most people realize. Current research indicates that this condition impacts roughly 10% of all women during their reproductive years – a staggering 190 million individuals globally, as reported by the World Health Organization. Despite its prevalence, countless women endure its symptoms in isolation, largely because their pain is frequently downplayed or misidentified as mere “normal period cramps.”
The Symptoms You Should Never Ignore
The most unmistakable indicator of endometriosis is pelvic pain that dramatically surpasses the discomfort of typical menstrual cramps. This isn’t just a fleeting ache; it can begin days before your period, intensify throughout its duration, and stubbornly persist even after your flow has ended. Sufferers often describe this agony as sharp, searing, or a deep, stabbing sensation—as if their internal organs are being squeezed tight, frequently accompanied by an overwhelming, flu-like malaise.
- Unusually heavy or unpredictable menstrual bleeding
- Excruciating pain during or immediately after sexual intercourse (dyspareunia)
- Significant discomfort or pain with bowel movements or urination, particularly intensified during your menstrual cycle
- Persistent, debilitating chronic fatigue that doesn’t improve with rest
- Unexplained bloating, persistent nausea, or other disruptive digestive problems that follow a cyclical pattern
- Challenges or difficulties with fertility and conception
Alarmingly, research reveals that between 30% and 50% of women diagnosed with endometriosis will encounter significant fertility challenges. While the struggle to conceive often brings women to seek medical help, it’s typically the relentless, unbearable pain that first prompts them to visit a doctor. If any of these symptoms resonate with your experience, understand this: you are absolutely not alone, and crucially, this pain is unequivocally *not* “all in your head.”
Real Women, Real Stories
Meet Sarah, a 32-year-old from Chicago, who endured years convinced she was just cursed with “unlucky periods.” Every single month, she’d miss work, abandon social engagements, and battle the crushing feeling that her own body was utterly failing her. Only after a diagnostic laparoscopy finally confirmed stage III endometriosis did she experience the profound relief of validation. “It wasn’t all in my head,” she tearfully recounts. With a personalized management plan in place, her pain significantly diminished, and she joyfully conceived her first child.
Then there’s Lisa, 28, who once collapsed in a grocery store, overwhelmed by excruciating pain. Her initial doctor visits yielded recommendations for stronger painkillers and advice to “just relax.” Years later, a crucial surgery unveiled severe endometriosis spread across her bowel and ovaries. “The sheer relief of finally putting a name to my suffering was indescribable,” she remembers. Once equipped with a precise care plan, her energy levels soared, and her overall mood dramatically improved.
These powerful accounts are far from isolated incidents. The heartbreaking reality is that the average delay in receiving an endometriosis diagnosis still hovers between a shocking 7 to 10 years. This prolonged suffering is frequently compounded by a societal narrative that subtly, or not so subtly, teaches women to downplay or simply “power through” their pain.
What Causes Endometriosis? Unraveling the Mystery
While medical researchers haven’t pinpointed a single, definitive cause for endometriosis, it’s widely understood that several interconnected factors likely contribute to its development. One prominent theory is “retrograde menstruation,” a phenomenon where menstrual blood, containing endometrial cells, flows backward through the fallopian tubes and into the pelvic cavity instead of exiting the body. Genetic predisposition also plays a significant role; if your mother or sister has endometriosis, your own risk of developing the condition is considerably heightened.
- Dysregulation or dysfunction within the immune system
- Significant hormonal influences, particularly elevated levels of estrogen
- Potential contributions from environmental factors, though more research is needed here
Crucially, it’s vital to understand that endometriosis is absolutely *not* caused by anything you did or failed to do. It is a profoundly complex medical condition, and recognizing this fundamental truth can alleviate the immense and unnecessary guilt that far too many women carry about their pain and diagnosis.
Why Early Awareness Matters More Than You Think
Leaving endometriosis untreated or inadequately managed can result in chronic inflammation and the relentless buildup of painful scar tissue, profoundly impacting every facet of daily life. Despite this, countless women delay seeking crucial help until their pain becomes utterly unbearable. Does this sound familiar: Have you ever had to cancel significant plans due to incapacitating period pain? Do you find yourself tracking your menstrual cycle with obsessive anxiety, dreading what’s to come? Or have you ever felt completely dismissed or invalidated when trying to articulate the severity of your symptoms to a healthcare provider?
Embracing early awareness, however, has the power to transform everything. It equips you with the confidence and knowledge to engage in truly informed conversations with your doctor, allowing you to initiate effective management strategies much sooner. The positive impact this can have on your overall quality of life is nothing short of profound.
Getting a Diagnosis: What You Need to Know
Unfortunately, there isn’t a single, straightforward blood test or imaging scan that can definitively diagnose endometriosis. While advanced ultrasounds and MRIs can be instrumental in spotting tell-tale cysts or deeper lesions, the undisputed gold standard for confirmation remains laparoscopy. This is a minimally invasive surgical procedure where a specialized surgeon carefully examines the pelvic cavity and takes tissue samples for biopsy, providing a conclusive diagnosis.
Please don’t let the idea of surgery intimidate you; for many women, receiving a definitive diagnosis through laparoscopy brings an enormous sense of relief and validation. To prepare for your appointment, begin meticulously tracking your symptoms: note the intensity of your pain, its exact timing in relation to your cycle, and its daily impact on your life. Bringing this detailed record to your doctor will provide them with a comprehensive picture, helping to accelerate your path to answers.
Effective Treatment Options That Offer Real Relief
While a definitive cure for endometriosis is still being sought, the good news is that its symptoms can often be managed with remarkable effectiveness. Because the condition manifests uniquely in each individual, collaborating closely with a gynecologist who possesses deep experience in endometriosis is absolutely crucial for crafting a successful treatment plan.
- Over-the-counter or prescription pain relief medications, including NSAIDs (nonsteroidal anti-inflammatory drugs)
- Various hormonal therapies, such as birth control pills, hormonal IUDs, or GnRH agonists, which work to reduce estrogen levels and inhibit the growth of endometrial tissue
- Surgical intervention, typically through laparoscopy, to meticulously remove endometrial lesions and adhesions
For optimal results, many women discover that a combination of medical treatments paired with supportive lifestyle adjustments yields the most significant improvements. It’s important to remember that what proves most effective is deeply personal and can vary considerably from one individual to another.
Empowering Lifestyle Strategies Many Women Swear By
While these strategies are not intended to replace professional medical care, incorporating these practical, supportive steps can significantly enhance your overall well-being and often provide tangible relief from symptoms for many women living with endometriosis.
- Embrace an anti-inflammatory diet rich in vibrant, colorful vegetables, abundant omega-3-rich foods such as wild salmon and walnuts, and consciously minimize processed foods and refined sugars.
- Incorporate gentle daily movement into your routine, whether it’s walking, restorative yoga, or swimming, to boost circulation and alleviate stiffness.
- Make prioritizing quality sleep a non-negotiable part of your day and actively integrate stress-reduction techniques like mindfulness or deep breathing.
- Apply targeted heat therapy to your lower abdomen during periods of intense pain to help soothe discomfort.
Using a straightforward period-tracking app can be an incredibly valuable tool, helping you identify recurring patterns in your symptoms and proactively prepare for those more challenging days.
When It’s Time to See a Doctor (Don’t Delay!)
If persistent pelvic pain is actively disrupting your career, straining your relationships, sabotaging your sleep, or impeding your daily activities—or if you’re struggling to conceive—it’s absolutely time to schedule a doctor’s appointment without delay. Remember to bring your meticulously kept symptom diary and be prepared to advocate for yourself with persistence. No one knows your body and its signals better than you do.
You might find yourself asking, “What if my symptoms aren’t actually endometriosis?” Seeking medical evaluation is crucial because, regardless of the diagnosis, getting answers will either confirm endometriosis or rule out other potential conditions, guiding you toward the precise support and treatment you need.
A Glimmer of Hope on the Horizon
Encouragingly, dedicated research is continuously advancing, focusing on developing superior diagnostic methods, innovative non-hormonal treatments, and even potential preventive strategies for endometriosis. Public awareness is steadily expanding, and a growing number of medical professionals are receiving specialized training to identify and address endometriosis earlier. Remember, you inherently deserve to feel heard, to receive clear answers, and to live a life filled with vitality instead of merely enduring the monthly cycle of pain.
Don’t Wait! Take Action Today with These Simple, Empowering Steps
- Immediately download a free, reliable period-tracking app and commit to logging your symptoms with complete honesty for at least the next two menstrual cycles.
- Proactively schedule an appointment with your gynecologist, or boldly request a referral to a specialist highly experienced in diagnosing and treating endometriosis.
- Share this vital article with a friend, family member, or anyone you suspect might benefit—openly discussing endometriosis helps to break the cycle of isolation and provides crucial support to others.
- Before your doctor’s visit, meticulously prepare a concise list of all your questions and concerns, ensuring you feel confident, empowered, and fully prepared to advocate for your health.
Do not resign yourself to enduring another agonizing cycle. Taking these small, deliberate actions today can pave the way for genuine, lasting relief and a significantly improved quality of life tomorrow.
Conclusion: Reclaim Your Life
In summary, endometriosis is a very real, profoundly impactful condition, and acquiring knowledge about it is your ultimate superpower. By learning to recognize its often-misunderstood symptoms, gaining a deeper understanding of the condition itself, and courageously taking proactive steps, countless women worldwide are now discovering effective strategies to manage their pain and decisively reclaim their lives. Let this resonate deeply: Your pain is undeniably valid. Your personal story holds immense importance. And crucially, effective help and unwavering support are absolutely available to you.
Frequently Asked Questions About Endometriosis
Is there a definitive cure for endometriosis?
Currently, there is no known cure for endometriosis. However, the good news is that its challenging symptoms can be managed very effectively through a combination of medications, targeted hormonal therapy, surgical interventions, and supportive lifestyle modifications. With the right personalized care plan, many women experience substantial and life-changing relief.
What is the typical timeframe for an endometriosis diagnosis?
The unfortunate reality is that, on average, it takes approximately 7 to 10 years to receive an endometriosis diagnosis. However, by diligently tracking your symptoms and actively seeking out a specialist with extensive experience in endometriosis, you can significantly accelerate this often-frustrating diagnostic journey.
Can adopting specific lifestyle changes truly help in managing endometriosis pain?
Absolutely, yes. While not a standalone solution, integrating an anti-inflammatory diet, engaging in gentle daily physical activity, actively practicing stress reduction techniques, and utilizing heat therapy can powerfully complement medical treatments, leading to a notable improvement in the quality of life for many women affected by endometriosis.
Please note: This article is intended solely for informational purposes and should never be considered a substitute for professional medical advice, diagnosis, or treatment. Always consult with your qualified healthcare provider for personalized guidance regarding your individual health concerns.