Ever wondered why that stubborn stomach ache just won’t quit, despite all your efforts? What if I told you a tiny, spiral-shaped bacterium, H. pylori, is silently residing in over half the world’s population, potentially causing that very discomfort – and you might be one of them without even knowing it? This isn’t just about fleeting indigestion; for millions, it’s a persistent, unsettling presence that quietly saps their energy and peace of mind. The good news? Unraveling the mysteries of this incredibly common infection can unlock practical strategies and medical solutions that truly transform your gut health. But don’t click away just yet, because I’m about to reveal a surprising truth about its easy spread and exactly what immediate steps you can take to safeguard your digestive system for good.
What Exactly Is Helicobacter Pylori?
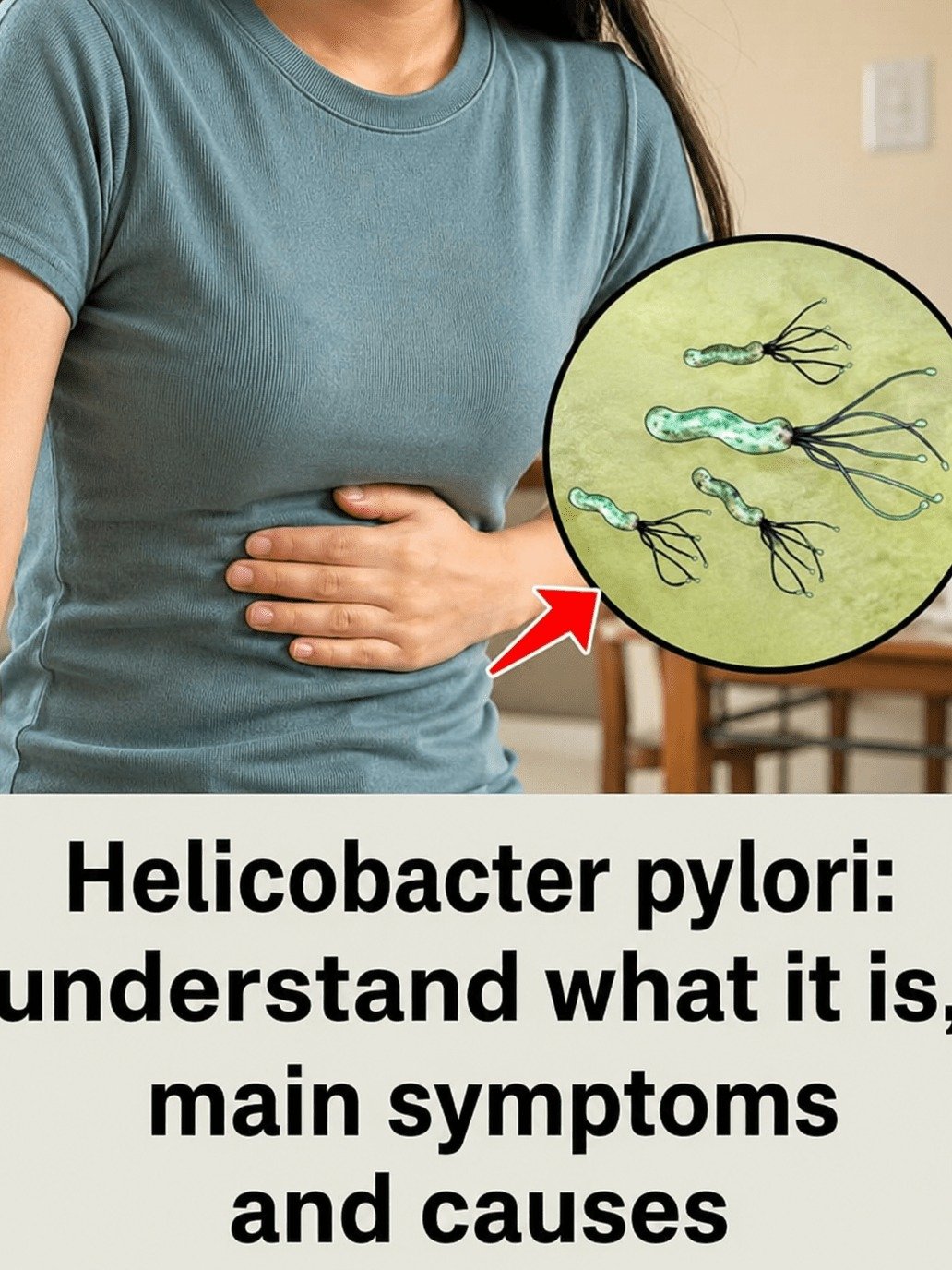
So, what exactly are we talking about when we say Helicobacter pylori? Also known as H. pylori, this isn’t just any ordinary germ; it’s a uniquely spiral-shaped bacterium that has mastered the art of thriving in the incredibly acidic conditions of your stomach. Renowned medical institutions like the Mayo Clinic and Cleveland Clinic confirm that it expertly latches onto the crucial mucous lining of your stomach and the duodenum, which is the initial segment of your small intestine, slowly igniting a low-grade inflammation that can build up over time.
The astonishing truth is that a significant number of individuals harboring this bacterium will never actually encounter any discernible issues. Indeed, extensive research highlights that countless H. pylori infections can lie completely dormant, remaining undetected for many years, sometimes even for decades. However, the moment this clever bacteria upsets the finely tuned equilibrium within your stomach, it can unleash an irritation that feels anything but trivial, demanding your attention.
What gives H. pylori its remarkable edge and sets it apart from other microorganisms? It’s all thanks to a specialized enzyme it produces, called urease. This enzyme works like a shield, effectively neutralizing the powerful stomach acid in its immediate vicinity, thereby creating a safe haven where it can flourish while other bacteria would simply be destroyed. This ingenious survival mechanism is precisely why H. pylori has managed to become one of the planet’s most pervasive and successful infections.
How Common Is H. Pylori and Who Gets It?
Just how prevalent is H. pylori, and who exactly is at risk? This bacterium is shockingly widespread, with worldwide projections indicating it impacts approximately 50% of all adults. You’ll typically find higher rates of infection in developing nations, as well as among communities facing crowded living situations or those with inadequate access to safe, clean drinking water. While the figures are somewhat lower in countries like the United States and other developed regions, the presence of H. pylori remains substantial, particularly within older demographics and specific ethnic communities.
Intriguingly, this infection often takes root during early childhood, and if left untreated, it has the potential to linger throughout an individual’s entire life. However, it’s crucial to understand that merely carrying the bacteria doesn’t automatically mean you’ll develop health problems; a considerable number of people coexist with H. pylori without experiencing any adverse symptoms whatsoever, living their lives feeling completely healthy.
However, prepare for a revelation that often catches people off guard: it’s incredibly common for H. pylori to be shared among family members and close household contacts. This happens precisely because of the intimate ways this bacterium manages to spread from one person to another.
How Does H. Pylori Spread from Person to Person?
So, how exactly does H. pylori make its way from one person to another? The primary pathway for transmission is through direct, close personal contact. This tenacious bacterium can readily transfer through bodily fluids such as saliva, vomit, or even stool. Often, this occurs during formative childhood years through seemingly innocuous daily interactions like sharing eating utensils, exchanging kisses, or simply due to inadequate handwashing practices following restroom visits. Additionally, consuming food or water that has been contaminated, especially in regions with less-than-ideal sanitation infrastructure, can also contribute significantly to its spread.
Once it successfully enters the body, experts at the Cleveland Clinic confirm that H. pylori skillfully navigates its way down to the stomach lining, where it establishes its long-term home. What’s particularly fascinating is the strong correlation between its prevalence and environmental factors: inadequate sanitation and densely populated living environments significantly amplify the likelihood of infection. This crucial insight helps us understand why infection rates fluctuate so dramatically across different global regions.
But there’s more to this story: ongoing research consistently reveals that exposure during early childhood represents the most frequent pattern of infection. This implies a startling reality – a considerable number of adults living today could have been carrying H. pylori since their youth, completely unaware, and never having linked these long-term residents to their current, often frustrating, stomach discomforts.
Recognizing the Symptoms of H. Pylori Infection
Identifying an H. pylori infection can be deceptively challenging because, for the vast majority of individuals, there are absolutely no noticeable symptoms. However, when signs do manifest, they typically arise as a direct consequence of the inflammation, known as gastritis, or the painful open sores, called peptic ulcers, that this bacteria is capable of inducing within the digestive tract.
- A persistent burning or gnawing sensation in the upper abdominal region, which can fluctuate but often intensifies when your stomach is empty
- Regular episodes of uncomfortable bloating or experiencing a profound sense of fullness even after consuming only small quantities of food
- Noticeably increased burping or belching that seems disproportionate
- Feelings of nausea or sporadic bouts of vomiting
- A noticeable decrease in appetite or unexplained, unintentional weight loss
- The appearance of dark, tar-like stools, which is a critical symptom demanding immediate medical evaluation
It’s important to recognize, as emphasized by reputable sources like WebMD and the Mayo Clinic, that these symptoms can unfortunately mimic those of numerous other digestive conditions. This significant overlap underscores precisely why obtaining a professional diagnosis through specific testing is absolutely crucial for accurate identification.
Should you find yourself consistently grappling with any of these challenging symptoms, please understand that you are far from alone in this experience. The truly encouraging news is that achieving a clear diagnosis can pave the way for genuine and lasting relief.
Potential Complications Worth Knowing
What happens if H. pylori goes unchecked? If the inflammation caused by H. pylori persists for several years without intervention, it can potentially escalate into painful peptic ulcers, forming either in the stomach itself or within the duodenum. Furthermore, in more infrequent scenarios, a prolonged infection has been scientifically associated with an elevated risk of developing specific types of stomach cancers or a particular form of lymphoma, a consensus firmly supported by leading medical bodies such as the CDC.
Essentially, this bacteria compromises your stomach’s vital protective lining, leaving it vulnerable to the corrosive effects of digestive acids, which can then etch out painful open sores. However, it’s vital to keep in mind that the overwhelming majority of individuals carrying H. pylori will never progress to these severe stages—emphasizing that proactive awareness and timely intervention are absolutely paramount.
How Doctors Diagnose H. Pylori
The good news is that securing an accurate diagnosis for H. pylori is generally a simple and often non-invasive process. Here are the most common diagnostic approaches:
- Urea breath test: This involves consuming a specialized solution, then exhaling into a collection bag – it’s a remarkably straightforward, rapid, and exceptionally accurate method.
- Stool antigen test: A laboratory analysis of a stool sample is performed to identify specific bacterial proteins, indicating the presence of H. pylori.
- Blood test: While it can detect antibodies, suggesting past exposure, this method is generally considered less reliable for confirming an active, current infection.
- Endoscopy with biopsy: This procedure is typically reserved for situations where symptoms strongly point towards ulcers, or when other serious gastrointestinal concerns warrant a direct visual examination and tissue sampling.
Your physician will carefully assess your individual health profile and symptoms to determine the most appropriate diagnostic test for you. The crucial message here is simple: these advanced tests are designed to deliver definitive answers, empowering both you and your healthcare provider to collaboratively chart the most effective course of action moving forward.
Treatment Approaches for H. Pylori
Should treatment be deemed necessary, the standard approach usually entails a powerful combination therapy: a course of antibiotics paired with acid-reducing medications, typically administered over a period of 10 to 14 days. Proton pump inhibitors (PPIs) play a vital role by significantly decreasing stomach acid levels, creating an environment where the antibiotics can more effectively eradicate the bacteria. Occasionally, bismuth compounds are incorporated into the regimen, offering an additional layer of protection and efficacy against the infection.
The good news is that success rates for H. pylori eradication are remarkably high, provided the entire course of medication is meticulously followed as prescribed. Given the potential challenge of antibiotic resistance, your doctor will often schedule a crucial “test of cure” a few weeks after treatment completion, typically utilizing a breath or stool test to definitively confirm that the infection has been successfully cleared.
For many, this is the most comforting aspect: collaborating closely with your doctor ensures you receive tailored, personalized care that perfectly aligns with your unique health history and current profile, optimizing your chances for a full recovery.
Actionable Tips You Can Start Today
Feeling proactive and eager to take control, whether you’re awaiting a medical appointment or have just completed one? Here are some highly actionable and practical steps you can implement starting today to bolster your overall digestive wellness:
- Commit to impeccable hand hygiene: always wash your hands meticulously with soap and water after using the restroom and before preparing or consuming any food.
- Consciously refrain from sharing personal items such as eating utensils, drinking glasses, or toothbrushes with other individuals.
- Prioritize consuming only safe, purified drinking water, particularly when you are traveling to unfamiliar areas.
- If you frequently experience post-meal discomfort, consider adopting a pattern of eating smaller, more frequent meals throughout the day.
- If you have a history of stomach sensitivities or issues, it’s wise to limit or completely avoid NSAIDs, like ibuprofen, as they can exacerbate gastric irritation.
Beyond these immediate actions, here’s an additional compilation of lifestyle adjustments that countless individuals have found remarkably advantageous for their gut health:
- Consider integrating probiotic-packed foods such as natural yogurt or kefir into your diet, but always consult with your doctor first.
- Actively manage your stress levels through calming practices like gentle exercise, mindfulness meditation, or ensuring you get sufficient, restorative sleep.
- If you are a smoker, making the decision to quit can significantly accelerate your body’s healing processes.
- Maintain optimal hydration by drinking plenty of water and, during periods of discomfort or flare-ups, choose bland, easily digestible foods.
While these supportive measures are not a substitute for professional medical treatment, they can undeniably enhance your daily comfort and overall well-being as you navigate your health journey.
Prevention Strategies That Actually Work
Effective prevention strategies are primarily centered on disrupting the transmission cycle of H. pylori. This involves a strong emphasis on cultivating excellent hygiene habits, consistently adhering to safe food and water consumption practices, and fostering heightened awareness within family units. In regions where the infection is particularly widespread, ongoing community education initiatives focused on improved sanitation have consistently demonstrated their ability to reduce the incidence of new cases over extended periods.
However, perhaps the single most potent preventive measure at your disposal is to remain vigilant: pay close attention to any persistent or unusual symptoms and proactively seek professional medical guidance at the earliest sign, rather than allowing the condition to escalate and worsen over time.
Wrapping It All Up
Coping with persistent, unexplained stomach discomfort can be an incredibly isolating and draining experience. Yet, armed with comprehensive knowledge about Helicobacter pylori, you gain the power to take decisive, informed action. From learning to identify its often-subtle symptoms and grasping how it spreads, to proactively seeking accurate diagnostic testing, each step you take moves you closer to experiencing profound relief and safeguarding your long-term health. While this bacterium is undeniably widespread, the clear path forward—forged through candid discussions with your doctor and the adoption of straightforward daily habits—is unequivocally within your grasp.
Frequently Asked Questions (FAQ)
Can H. pylori infection go away without treatment?
While certain mild infections might indeed lie dormant for extended periods, it’s exceptionally rare for the H. pylori bacteria to spontaneously vanish entirely from the body on its own. The consensus among most medical professionals is to strongly advise a thorough medical evaluation if any symptoms begin to manifest.
Is H. pylori contagious?
Absolutely, H. pylori is indeed contagious. It primarily spreads through direct person-to-person contact or via exposure to contaminated food and water sources. Implementing rigorous hygiene practices is a highly effective way to significantly minimize the risk of transmission within family environments and households.
How long does treatment for H. pylori usually take?
Typically, the standard course of treatment for H. pylori spans a duration of 10 to 14 days. Following the completion of your medication, your physician will arrange for follow-up testing to definitively confirm that the treatment regimen has been successful in eradicating the infection from your system.
Disclaimer: Please note, the content presented in this article is provided strictly for educational and general informational purposes. It should not, under any circumstances, be interpreted as a substitute for professional medical advice, a formal diagnosis, or a prescribed treatment plan. It is imperative that you always seek the personalized guidance of a qualified healthcare professional concerning any symptoms or health-related concerns you may have. Be aware that individual outcomes and specific medical recommendations can fluctuate significantly based on your unique medical history and current health status.
(Word count: approximately 1,320)