Picture this: you spot a peculiar red circle on your skin, maybe on your hand or arm. Initially, you might brush it off as a simple dry patch or an allergic reaction, but then the itch intensifies, the edges begin to rise and flake, and suddenly, it’s multiplying. A wave of panic washes over you – is this contagious? Will it get worse? Could it be something serious that demands immediate attention? The discomfort and self-consciousness can quickly turn everyday activities into a frustrating ordeal. The good news is that deciphering these specific skin signals can lead you to clarity and relief far sooner than you might think. But here’s the critical part: there’s a surprising, often overlooked detail that can dramatically accelerate your recovery and get your skin back to normal.
What Those Red Circular Rashes Actually Look Like
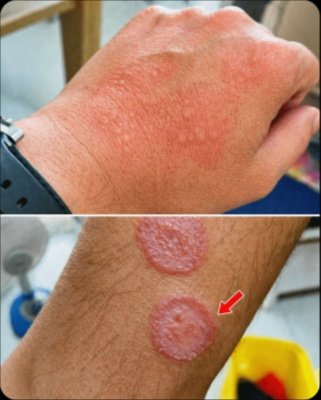
When you examine common images of this particular skin condition, often shared by individuals experiencing it, two primary visual presentations frequently stand out. One pattern typically presents as a broad area of redness and dryness, commonly observed on the back of the hand. The second, and perhaps more classic, manifestation features distinct ring-shaped lesions on areas like the forearm—precisely the kind often emphasized in patient photos—characterized by elevated, inflamed edges and frequently a noticeably clearer area in the very center. These aren’t merely arbitrary blemishes; they adhere to a precise and recognizable configuration that skin specialists can identify almost instantly.
The Most Common Culprit: Ringworm (Tinea Corporis)
Don’t let the alarming name fool you: ‘ringworm’ has absolutely nothing to do with worms. Instead, it’s a common fungal skin infection, medically known as tinea corporis, caused by a group of fungi called dermatophytes. Extensive research from leading dermatology organizations consistently highlights that these fungi flourish in environments that are both warm and moist, and they are notoriously easy to transmit through direct physical contact.
Key Signs That Point to Ringworm
When professionals suspect ringworm, these are the unmistakable, classic indicators they are trained to identify:
- Distinct ring-shaped or perfectly circular red patches, often featuring sharply defined, elevated, and scaly borders.
- A noticeable central clearing, giving the lesion its characteristic ring-like appearance, much like a target.
- Persistent and intense itching, which can become severe enough to significantly interfere with sleep and daily routines.
- The emergence of spreading or multiple lesions across various body parts, including hands, arms, legs, or the torso.
- Presence of slight scaling or subtle crusting, predominantly along the lesion’s edges.
However, it’s important to note that the presentation isn’t always textbook. Occasionally, this infection can manifest with a more diffuse and generalized inflammation, particularly noticeable on the hands. This broader redness often aligns with the initial widespread irritation many individuals first observe on their skin.
Other Conditions That Can Look Almost Identical
This is where the plot thickens: not every red, circular mark on your skin points to ringworm. In fact, a number of other prevalent skin conditions can astonishingly resemble it, making accurate self-diagnosis incredibly challenging.
- Nummular (discoid) eczema: These are distinct, coin-shaped, and intensely itchy patches that frequently emerge following a skin injury or in environments with low humidity.
- Granuloma annulare: Characterized by smooth, ring-like bumps, these lesions are typically devoid of pain and often resolve spontaneously without intervention.
- Contact dermatitis or psoriasis plaques: While capable of forming circular designs, these conditions generally present with unique textures or are triggered by distinct factors compared to ringworm.
This intricate overlap of symptoms clearly illustrates why attempting to self-diagnose can so easily steer you in the wrong direction, potentially delaying effective treatment. The reassuring news, however, is that a brief consultation with your healthcare provider can swiftly clarify the situation, often through a straightforward skin scraping or a thorough visual examination.
What Triggers These Rashes in the First Place?
Fungal infections, by their very nature, thrive in conditions of warmth, moisture, and close proximity. Consistent research data unequivocally points to elevated incidence rates in humid regions, among individuals who participate in sports, and within homes where pets are carriers of the fungus. Key risk factors that increase your susceptibility include:
- Regularly sharing personal items such as towels, gym apparatus, or articles of clothing.
- Engaging in strenuous, sweaty workouts and failing to change out of damp attire immediately afterward.
- Having a weakened immune system or undergoing a recent course of antibiotics.
- Direct and intimate contact with either infected individuals or animals.
Identifying and acknowledging your specific personal triggers is, without a doubt, one of the most effective and rapid strategies for breaking the cycle of these recurring infections.
Actionable Tips: What You Can Do Right Now (Step-by-Step)
You are not powerless in this situation; there are immediate, proactive steps you can take. Here’s a straightforward, step-by-step action plan you can implement starting today, even as you arrange for a professional medical consultation:
- Maintain immaculate cleanliness and dryness in the affected area — Gently cleanse the skin using a mild, fragrance-free soap, ensuring it is thoroughly patted dry. Crucially, refrain from covering it with restrictive clothing or bandages.
- Effectively manage the itch to prevent further spread — Apply cool compresses to soothe the skin and, most importantly, resist the urge to scratch, which can lead to secondary bacterial infections.
- Explore suitable over-the-counter remedies — For suspected fungal infections, topical antifungal creams might offer relief (consult your pharmacist for product recommendations tailored to your symptoms), but discontinue use if you notice increased irritation.
- Safeguard both yourself and those around you — Launder all bedding, towels, and clothing in hot water, and strictly avoid sharing any personal items until your condition has completely cleared.
- Monitor and document daily changes — Take dated photographs of the rash regularly. This visual record will be invaluable for your doctor to accurately assess its progression.
The single most crucial action you can take? Schedule that appointment with a dermatologist or your primary care physician without delay. Prompt intervention nearly always translates into a quicker, less complicated resolution to your skin concerns.
Smart Prevention Strategies to Keep Rashes Away for Good
When it comes to skin health, proactive prevention is consistently a far simpler and more effective approach than reactive treatment. Incorporating these straightforward daily habits can yield a monumental difference in keeping these rashes at bay:
- Always change out of any sweaty clothing as soon as you complete your exercise routine.
- Opt for breathable fabrics and make a conscious effort to keep your skin as dry as possible, especially during periods of high humidity.
- Under no circumstances should you ever share personal hygiene items such as razors, towels, or even your gym equipment.
- Regularly inspect your household pets for any signs of hair loss or scaly patches, and seek veterinary treatment for them without delay if symptoms appear.
Numerous studies unequivocally demonstrate that maintaining consistent and diligent hygiene practices plays a significant role in drastically reducing the likelihood of experiencing recurring fungal skin issues.
When Should You See a Doctor Immediately?
It is imperative not to delay seeking medical attention if your rash begins to spread rapidly, escalates in pain, starts to ooze, or if you experience accompanying symptoms like a fever or swollen lymph nodes, or if there’s no noticeable improvement within a week. Individuals with underlying conditions such as diabetes, compromised immune systems, or those with extensive skin involvement are particularly urged to seek immediate professional care.
Conclusion: Your Skin Is Trying to Tell You Something
Ultimately, those distinct red circular patches are not just blemishes; they are your body’s unmistakable signals, urging you to pay attention. By learning to recognize these signs early, implementing effective practical measures, and seeking expert medical guidance when necessary, the vast majority of individuals can achieve remarkable improvement and restore their confidence in their skin’s health. Remember that surprising secret we hinted at right from the start? It’s simply this: the more swiftly you act upon accurate information and appropriate care, the less time you will spend grappling with discomfort – and the sooner you can shed that worry and reclaim a life of comfort and peace of mind.
Frequently Asked Questions
1. Is every red circular rash inherently contagious?
Absolutely not. While ringworm is indeed transmissible, numerous other conditions that bear a striking resemblance to it, such as nummular eczema or granuloma annulare, are not contagious. A definitive diagnosis from a qualified healthcare professional is essential to differentiate between them.
2. What is the typical timeline for these rashes to clear up?
With diligent and appropriate management, many individuals observe noticeable improvements within a span of 1 to 2 weeks. However, complete resolution can extend beyond this, depending significantly on the underlying cause and the promptness with which treatment commenced. Always adhere strictly to your doctor’s personalized advice.
3. Is it possible to completely treat a suspected ringworm rash using only home remedies?
While some mild instances might show a response to readily available over-the-counter antifungal products, attempting self-treatment carries the inherent risk of misdiagnosis, employing an ineffective approach, or inadvertently delaying the necessary professional care. Consulting a medical expert ensures you receive the correct diagnosis and the safest, most effective treatment for the actual cause of your rash.
Disclaimer: This article is provided strictly for informational purposes and should never be considered a replacement for professional medical advice, accurate diagnosis, or prescribed treatment. It is always crucial to consult your personal healthcare provider or a dermatologist regarding any skin concerns or notable changes in your health. Please be aware that individual results from treatments or advice may vary.