Imagine feeling that familiar tingle, knowing exactly what’s coming next: another round of painful, embarrassing blisters on your lips or private areas. This isn’t just a ‘bad luck’ skin issue; it’s your body sending a clear, urgent message that most people completely misunderstand. For years, you might have felt trapped in a frustrating cycle, wondering why these recurrent outbreaks keep sabotaging your confidence and intimate moments, despite every cream or home remedy you’ve tried. The truth is, this persistent pattern is significantly more prevalent than you might think, and it’s often a direct signal from your body about a specific viral process, not merely a random skin irritation.
Why These Recurrent Blisters Are Not “Just a Skin Thing”
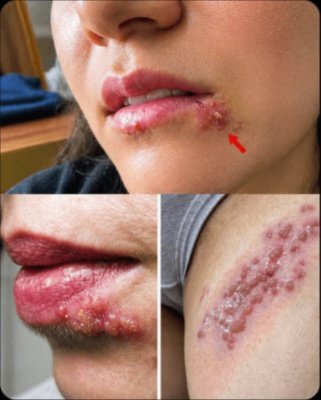
Let’s be clear: those recurring blisters in such sensitive spots are almost always a tell-tale sign of the herpes simplex virus (HSV), which can manifest as bothersome cold sores around the mouth or uncomfortable lesions in the genital area. Once this virus enters your system—often through an initial infection so mild it goes unnoticed—it retreats into your nerve cells, lying in wait. It remains dormant until specific triggers stir it back to life. Astonishingly, data from health authorities like the CDC reveals that a substantial percentage of adults harbor either HSV-1 or HSV-2, yet a surprising number are completely unaware, thanks to symptoms that can be either very subtle or entirely absent between flare-ups.
Here’s the critical insight many overlook: each recurrence isn’t just a random event; it’s your body’s specific alarm system, signaling that the virus has reactivated and is traveling along its established nerve pathways. Scientific studies consistently show that a staggering 70–90% of individuals carrying the virus will experience these repeat episodes, even though the frequency can differ greatly from person to person. The truly empowering news? Grasping this underlying pattern unlocks a powerful arsenal of practical strategies that can profoundly diminish both the frequency and intensity of future outbreaks.
Understanding the Hidden Reality Behind Recurrent Outbreaks
During a typical, fast-paced doctor’s appointment, what often goes unsaid is that while HSV can indeed be a lifelong presence for many, it absolutely doesn’t have to dictate your life or calendar. The mechanism is fascinating: the virus makes its journey back down the nerves to the skin or mucous membranes precisely when your immune system’s vigilance momentarily weakens. This perfectly accounts for the well-known progression of an outbreak: that initial tingling sensation (known as the prodrome), followed by redness, the emergence of tiny clusters of fluid-filled blisters, their eventual bursting, crusting over, and finally, healing within a typical timeframe of 7 to 14 days.
So, why is this crucial for you to understand, right now? Because these recurrent episodes reach far beyond mere skin discomfort; they frequently cast a shadow over your emotional well-being, strain relationships, and erode self-esteem. However, groundbreaking modern approaches, centered on heightened awareness and robust support, have empowered countless individuals to transform their experience, moving from the monthly dread of outbreaks to enjoying rare, significantly milder episodes.
Yet, there’s an even deeper layer to this story. Specific, common everyday factors possess the power to coax the dormant virus out of its hiding place. Extensive research consistently points to several primary culprits that almost every individual will encounter at some point in their lives. The profound act of recognizing and understanding your own unique trigger patterns stands as one of the most empowering and proactive steps you can possibly take.
Let’s uncover some of the most widely reported and impactful triggers:
- Stress and emotional strain — When your body is under pressure, elevated cortisol levels can compromise your immune system, making it a prime time for an outbreak to emerge.
- Sun exposure or UV light — Particularly on the lips, intense UV rays can irritate the delicate nerve endings, acting as a direct trigger.
- Hormonal shifts — Significant fluctuations, common during menstruation or pregnancy for women, can create an environment conducive to reactivation.
- Illness or fatigue — Battling a cold, fever, or enduring insufficient sleep can critically lower your body’s natural defenses, leaving you vulnerable.
- Physical trauma or friction — Even slight physical irritation or friction, especially in sensitive areas like the genitals, can provoke an outbreak.
Diligently tracking these factors over just a few months will frequently illuminate your specific combination of triggers, equipping you with the vital knowledge to implement truly proactive prevention strategies.
The Prodrome Phase: Your Body’s Early Warning System
Now, for one of the most intriguing and empowering aspects. That unmistakable tingle, itch, or burning sensation that surfaces a full 12–48 hours before any visible blisters emerge is known as the prodrome phase. This isn’t just a symptom; it’s your body’s invaluable early warning system, offering a crucial window of opportunity to intervene. Clinical observations confirm that taking action swiftly during this prodromal stage can significantly shorten the duration of an outbreak and dramatically lessen its severity.
Actionable Tips: 5 Practical Steps You Can Start Today
You absolutely do not have to passively wait for the next episode to strike to reclaim a sense of control. These proven, evidence-based strategies, when integrated with expert professional guidance, are designed to help you not only manage symptoms more effectively but also significantly reduce the frequency of future recurrences:
- Track your patterns diligently — Start a straightforward journal where you log stress levels, dietary choices, sleep quality, your menstrual cycle (if relevant), and sun exposure in the days leading up to each episode. Within just 3 months, your unique patterns will typically become strikingly clear.
- Fortify your immune system every single day — Make consistent, quality sleep (aiming for 7–9 hours) a top priority. Fuel your body with a balanced diet abundant in fresh fruits and vibrant vegetables, and integrate stress-reduction techniques such as brief daily walks or mindfulness meditation into your routine.
- Proactively guard against identified triggers — Always apply a lip balm containing SPF before any sun exposure. Additionally, opt for loose-fitting clothing to minimize friction in sensitive areas, particularly during times you anticipate or experience active periods.
- Engage with a healthcare provider without delay — If you’re experiencing frequent outbreaks, it’s vital to discuss options for prescription antiviral medications. Extensive research unequivocally demonstrates that these can reduce recurrences by a significant margin, whether used episodically at the first sign of an outbreak or daily as suppressive therapy.
- Embrace open communication — When you feel prepared, having honest conversations with partners about your experiences can not only alleviate personal anxiety but also foster safer and more understanding intimacy choices.
Countless individuals discover that by consistently integrating these daily habits with personalized medical advice, they experience remarkable and noticeable improvements within a matter of months.
Comparing Recurrent Outbreaks: What Changes With Better Management
To truly underscore the transformation available to you, let’s take a compelling side-by-side look at the typical experience without informed management compared to the profound possibilities that open up when you take proactive, educated steps:
| Aspect | Common Experience Without Targeted Management | With Consistent Awareness and Professional Support |
|---|---|---|
| Frequency | Every 1–6 months | Often reduced to 0–2 times per year |
| Severity & Duration | Painful blisters lasting 7–14 days | Milder symptoms resolving in 3–7 days |
| Emotional Impact | Heightened anxiety and self-consciousness | Greater confidence and reduced worry |
| Daily Disruption | Frequent need to cover up or avoid activities | More predictable and manageable episodes |
This insightful comparison draws directly from general patterns and outcomes consistently reported in both rigorous clinical studies and real-world patient experiences.
Real Stories That Show Change Is Possible
Consider Sarah, a 34-year-old professional who endured debilitating genital outbreaks every 6–8 weeks, predictably triggered by high stress levels and her menstrual cycle. However, after she became adept at recognizing her prodrome symptoms and collaborated with her doctor on a tailored management plan, her episodes plummeted dramatically. Inspiring stories like Sarah’s serve as a powerful testament that genuine knowledge is the ultimate catalyst, transforming the experience from one of quiet shame into profound empowerment.
Breaking the Cycle: What Science Supports
But hold on—the journey to control doesn’t end there; in fact, there’s even more you can actively do. Emerging research suggests that key lifestyle factors, such as diligently maintaining healthy levels of vitamin D and zinc (always in consultation with your doctor), play supportive roles in bolstering overall immune resilience. The absolute key here is unwavering consistency and utterly rejecting the pervasive myth that you must simply ‘live with it’ indefinitely.
Conclusion: Taking Back Control Starts With Understanding
Ultimately, those recurrent rashes or blisters appearing on your lips or private areas are far from something to ignore or endure in silence. They are, in fact, a remarkably common signal that your body is actively managing a virus that a vast majority of adults will encounter at some point in their lives. By astutely recognizing your unique patterns, pinpointing individual triggers, and forging a proactive partnership with a trusted healthcare professional, you can decisively shift towards experiencing significantly fewer disruptions and cultivating a profound sense of peace. This cycle does not, and will not, have to define who you are.
Frequently Asked Questions
1. Is there a permanent cure for recurrent herpes-related blisters?
While a permanent cure for the virus itself remains elusive at present, a vast number of individuals successfully manage their symptoms and dramatically reduce outbreak frequency through a combination of thoughtful lifestyle adjustments and proven medical options, always discussed with their doctor.
2. How can I tell if my blisters are from HSV versus another condition?
It’s crucial to understand that only a qualified healthcare provider can definitively confirm whether your blisters are due to HSV or another condition through proper testing. Given that similar symptoms can arise from various causes, early evaluation is strongly recommended for accurate diagnosis and tailored guidance.
3. Does having recurrent outbreaks mean I’m more likely to transmit it to others?
It’s true that transmission risk exists even during periods without visible symptoms (a phenomenon known as asymptomatic shedding). However, by diligently implementing consistent management strategies and engaging in open, honest conversations with your partners, you can significantly lower that risk and foster responsible intimacy.
Disclaimer
This article is for informational and educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult a qualified healthcare provider regarding any health concerns or before starting any new regimen. Individual results may vary.